Introduction
Mental health is an incredibly important issue affecting a significant number of Australians – nearly 1 in 2 Australians will experience a mental health disorder in their lifetime. Whilst external factors such as stress and environment of course contribute to poor mental health, Changes in our physical health can also impact our mood and may even contribute to or worsen mental health conditions. The importance of our gut microbiome for gastrointestinal health is something that is well established – many of us are aware of the benefits of probiotics for supporting healthy digestion. But how does our microbiome affect other areas of our health, such as our mood? There is growing evidence to support an important link between our microbiome and our mood – the microbiome may have an important role to play in not only helping us to feel happier, but even for helping to support those with mental health conditions such as depression, insomnia, and anxiety. In this blog, we examine the link between our gut, microbiome, and mood, and look at ways to support a healthy gut from a naturopathic perspective.
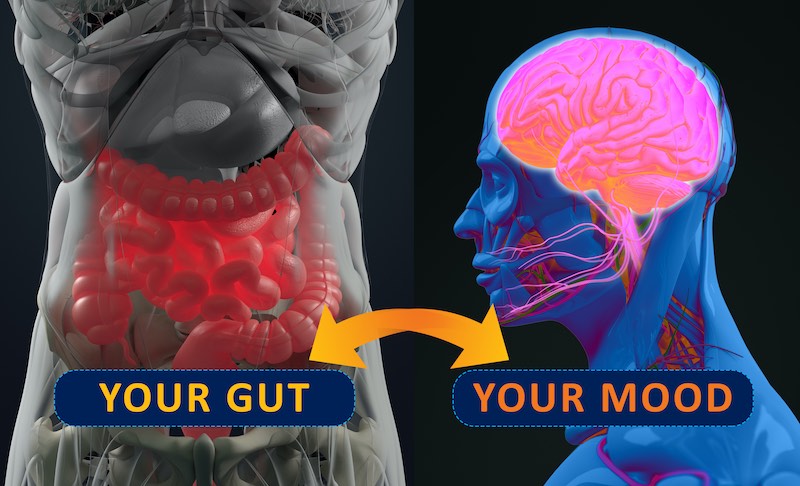
The Microbiome and The Gut-Brain Axis
The term “microbiome” or “gut microbiota” refers to the trillions of bacteria and other microorganisms that naturally live inside our intestines. We each have around 100 trillion bacteria, made up of approximately 100 different species, living inside our intestinal tract. The exact composition of each of our microbiomes is individual and depends on a range of factors, including genetics, geographic location, diet, and the use of medications, such as antibiotics.
One of the key connections between our microbiome and our mental health is through the gut-brain axis, a two-way communication pathway between our brains and our intestinal tract. This communication highway is mediated by the Vagus nerve, a large nerve that runs up through the centre of the abdomen. Microbes are able to send signals to the brain by directly and indirectly stimulating the Vagus nerve in various ways, but particularly through their ability to produce chemical messengers that send signals to the brain via this nerve. Certain bacteria inside our intestines produce significant amounts of neurotransmitters that are important for our mental health, including serotonin (the “happiness” molecule). In fact, 90% of our body’s circulating serotonin is produced not in the brain, but in our guts by intestinal bacteria, so microbes are playing a bigger role in your mood than you might think! Other important neurotransmitters such as dopamine, noradrenaline, GABA, and acetylcholine, can also be produced by intestinal bacteria. These chemicals play important roles in regulating our mood, anxiety, and even cognitive function.
Our intestinal microbes also influence inflammation levels inside the gut, as well as maintaining normal intestinal wall integrity (i.e. they help to prevent “leaky gut”). This is important, because both inflammation and leaky gut syndrome have been associated with mental illnesses such as depression. Changes in the make-up of the microbiome can lead to an increase in the production and release of inflammatory molecules called lipopolysaccharides. These and other inflammatory molecules send signals via the Vagus nerve up to the brain, causing changes in the brain that can induce symptoms of depression and anxiety.

So, how is the microbiome involved in specific mental health conditions?
Microbiome and Stress
Our microbiome influences how we perceive and react to stress in our lives. Stress leads to changes in the microbiome and can contribute to “dysbiosis” (an unhealthy imbalance of microbes in the gut). Animal studies have shown that a healthy gut microbiome actually helps to regulate our fight-or-flight response (also known as the HPA axis), meaning we are better able to cope with stressors in our lives when our microbiome is healthy.
Microbiome and Depression/ Anxiety
Inflammatory chemical messengers from bacteria have been shown to trigger symptoms of both depression and anxiety. Several studies have found that the types of intestinal bacteria present in the guts of people with major depressive disorder differs to that of the general population. However, there currently isn’t any consensus on any single bacteria that may be causing this link.
Microbiome and Insomnia
Recent research suggests that changes to the microbiome may play a role in insomnia, too. Studies have shown that interfering with normal sleep patterns (such as during shift work) can trigger changes to the intestinal microbiome. Another interesting role of the microbiome in influencing our sleep is in relation to our circadian rhythm, the internal clock that helps us to be awake and alert in the day, and sleepy at night. Studies on the microbiome show that the microbes within our intestines also follow a day-night pattern, fulfilling different functions depending on the time of day or night.
Supporting Your Mood and Your Gut Health
What can you do to help improve your mood and support your gut health? The following provides some tips on supporting both your mental wellbeing and your microbiome.
Eat a healthy diet:
- Certain dietary patterns, such as the Mediterranean Diet, have been shown to improve mental health and also provide lots of the types of foods that are good for supporting a healthy microbiome, too
- Reduce your intake of foods that preferentially feed unhealthy bacteria species – these foods include high sugar foods like cakes, lollies, and soft drinks, as well as foods high in trans fatty acids such as deep-fried foods
- Eat plenty of fibre-rich foods such as fruits, vegetables and wholegrains – Our “good” bacteria feed off of the complex carbohydrates found in these foods
- Our blog on feeding and nourishing your microbiome might also provide important tips https://www.performanceinhealth.com.au/2020/06/11/microbiome-family-gut-health/
Supplement with a high-quality probiotic:
- If you have recently taken medications such as antibiotics, have had a digestive issue such as diarrhoea, or have been through a period of significant stress, your microbiome may well benefit from a boost with a probiotic supplement
- Studies show that supplementing with probiotics can help to improve your mental health. Probiotics have been shown to increase serotonin levels, and clinical trials have shown that just 8 weeks of supplementation can cause marked improvement in symptoms of patients with depression. Other studies show that they are even effective when used in combination with prescribed anti-depressant medications
- The quality of probiotic supplements available on the market varies significantly, so it’s a good idea to discuss your needs with a naturopathic practitioner before beginning supplementation. Naturopaths are able to make recommendations to suit your individual health needs and ensure you are using a quality supplement that will benefit your health due to their extensive studies in this particular field.
Reduce your stress levels:
- As we’ve seen above, stress can affect our microbiome and our mental health, so reducing stress levels where possible is an important strategy for supporting mental wellbeing.
- Regular meditative practices such as yoga and mindfulness are well known for their stress-relieving abilities – check out your local yoga studio, or look into the many free apps that are available if you’d prefer to practice solo
- 20-30 minutes of daily exercise (such as a brisk walk through the neighbourhood) can also help to reduce stress
- Consider seeking the help of a counsellor or psychologist if you feel your stress would be better managed through talk therapy
Consider using herbal medicines:
- Bitter herbs such as gentian can be used before main meals to help improve your digestion and improve the pH in your intestines, which will help to help keep good bacteria happy
- Depending on your specific health needs, herbs such as liquorice, calendula, and chamomile might be beneficial by helping to soothe and heal any inflammatory damage in the intestines caused by dysbiosis
- As always, it is important to seek expert guidance from naturopathic practitioners before using herbal medicines. As a trained herbalist, a naturopath can assess your needs and create a unique blend that will work to best support your healing journey
It is important to remember that everyone’s digestion is unique. In working with many individuals with Irritable Bowel Syndrome (IBS), strategies to build a balanced microbiome may be more complicated initially and may require a restriction on certain prebiotic foods and low FODMAP food sources. For this reason, seeking one on one guidance is always recommended.
References
Australian Institute of Health and Welfare. (2021). Mental health. https://www.aihw.gov.au/reports/australias-health/mental-health
Bravo, J. A., Forsythe, P., Chew, M. V., Escaravage, E., Savignac, H. M., Dinan, T. G., Bienenstock, J., & Cryan, J. F. (2011). Ingestion of Lactobacillus strain regulates emotional behaviour and central GABA receptor expression in a mouse via the vagus nerve. PNAS, 108(38), 16050–16055. https://doi.org/10.1073/pnas.1102999108
Clapp, M., Aurora, N., Herrera, L., Bhatia, M., Wilen, E., & Wakefield, S. (2017). Gut microbiota’s effect on mental health: The gut-brain axis. Clinics and Practice, 7(987).
Desbonnet, L., Garrett, L., Clarke, G., Bienenstock, J., & Dinan, T. G. (2008). The probiotic Bifidobacteria infantis: An assessment of potential antidepressant properties in the rat. Journal of Psychiatric Research, 43(2), 167–174. https://doi.org/10.1016/j.jpsychires.2008.03.009
Du, Y., Gao, X.-R., Peng, L., & Ge, J.-F. (2020). Crosstalk between the microbiota-gut-brain axis and depression. Heliyon, 6. https://doi.org/10.1016/j.heliyon.2020.e04097
Hechtman, L. (2012). Clinical naturopathic medicine. Elsevier Australia.
Li, Y., Hao, Y., Fan, F., & Zhang, B. (2018). The role of microbiome in insomnia, circadian disturbance and depression. Frontiers in Psychiatry, 9.
Li, Y., Zhang, B., Zhou, Y., Wang, D., Liu, X., Li, L., Wang, T., Zhang, Y., Jiang, M., Tang, H., Amsel, L. V., Fan, F., & Hoven, C. W. (2020). Gut microbiota changes and their relationship with inflammation in patients with acute and chronic insomnia. Nature and Science of Sleep, 12, 895–905.
Limbana, T., Khan, F., & Eskander, N. (2020). Gut microbiome and depression: How microbes affect the way we think. Cureus, 12(8). https://doi.org/10.7759/cureus.9966
Liskiewicz, P., Kaczmarczyk, M., Misiak, B., Wronski, M., Baba-Kubis, A., Skonieczna-Zydecka, K., Marlicz, W., Bienkowski, P., Misera, A., Pela-Wysiecka, J., Kucharska-Mazur, J., Konopka, A., Loniewski, I., & Samochowiec, J. (n.d.). Analysis of gut microbiota and intestinal integrity markers of inpatients with major depressive disorder. Progress in Neuropsychopharmacology & Biological Psychiatry. https://doi.org/10.1016/j.pnpbp.2020.110076
Morkl, S., Wagner-Skacel, J., Lahousen, T., Lackner, S., Holasek, S. J., Bengesser, S. A., Painold, A., Holl, A. K., & Reininghaus, E. (2020). The role of nutrition and the gut-brain axis in psychiatry: A review of the literature. Neuropsychobiology, 79, 80–88.
Nikolova, V., Zaidi, S. Y., Young, A. H., Cleare, A. J., & Stone, J. M. (2019). Gut feeling: Randomized controlled trials of probiotics for the treatment of clinical depression: Systematic review and meta-analysis. Therapeutic Advances in Psychopharmacology, 9.