The dreaded ‘M’ word. Whilst our attitude to ageing is slowly changing, menopause remains a taboo topic, and for many it is still seen as the dreaded beginning of the decline into old age and even the end of productive life. However, with the average age of menopause being 51, many of us will spend around one third of our lives in this post-menopausal state. It certainly isn’t the decline into old age that it has been framed as! Far from being some dreaded phase to be avoided, menopause can be embraced as being a positive transition, a step forward in the journey of life and into a new phase of a full and vital life. Indeed, whilst menopause in Western society is often framed as being something negative to be persevered, many other societies around the globe embrace it as being a positive, natural transition in a woman’s life. Interestingly, perimenopausal symptoms in these societies are typically less troublesome! So, what exactly happens to the body after menopause, and how can we support ourselves for a healthy, positive transition to post-menopausal life? In this blog post we look at some of the physical and emotional changes associated with menopause and how a healthy post-menopausal life can look.
What is Menopause?
Menopause is quite simply the end of menstruation. It is diagnosed retroactively, one year after your final period. This means that if you are the right age and have been experiencing perimenopausal symptoms, then one year after your last menstrual period you are deemed as having entered menopause one year ago. In Western society, menopause is something which is diagnosed and treated, which frames menopause as some kind of disease, disorder, or deficiency. However, the truth is that menopause is none of these things. Much like puberty, menopause is simply a normal transition and a part of life – the shift to post-reproductive life.
What is Perimenopause?
Perimenopause is the time that precedes menopause. This is the period of 2-10 years before menopause where women typically experience “menopausal” symptoms – hot flashes, weight gain, irregular periods, night sweats, insomnia. It is a transitional phase as the body shifts and adapts to a state of lower oestrogen. For some women, perimenopause is a long, drawn-out time full of difficult to manage symptoms. For others, it is brief and relatively easy to cope with. If you’d like to learn more about perimenopause and the symptoms associated with this phase of life, see our blog post here.
Hot Flushes
One of the most frequent complaints of women during perimenopause is hot flushes, however within a few years of reaching menopause these resolve for the majority of women. For a minority of women hot flashes can continue into menopause and a more detailed review of causes is recommended so that you can reduce these symptoms.
What happens to the body after Menopause?
Interestingly, menopause still occurs at around 50 years of age even despite our longer life expectancies in modern times, which researchers believe suggests that longevity of our ovarian function is predetermined and possibly genetic. At birth, females have around 500,000 eggs in their ovaries, but this number declines throughout their lives. The rate of loss accelerates from around our mid-30s in the lead up to the perimenopausal period in our 40s.
The majority of the oestrogen in our bodies up until menopause is produced by the ovaries. After menopause, oestrogen levels significantly decline, because the ovaries are no longer producing any. Small amounts of oestrogen are still produced elsewhere in the body such as the adrenal glands, and fat cells convert androgens (“male” hormones made in the adrenal glands) into oestrogen, however this is a much weaker type of oestrogen than the ovaries produced. Progesterone levels also decline because of the loss of ovarian function. Small amounts of a weaker type of oestrogen are still produced in the adrenal glands, and fat cells convert some androgens (“male” type hormones) into weak oestrogen, too. The overall effect of this is that the body shifts into a low-oestrogenic state, and it is this significant change in our hormonal balance that triggers perimenopausal symptoms.
Oestrogen is a vitally important hormone that performs many, many functions in the body during the reproductive years, beyond simply being involved in ovulation and the menstrual cycle.
In fact, oestrogen is involved in many different functions, including the following:
- Maintains bone density by promoting osteoblast (bone-building) cell function
- Protects against heart disease via a range of complex mechanisms
- Improves cognition and protects against dementia by improving blood flow to the brain and helping certain brain cells to function
- Supports mental wellbeing by increasing serotonin production
Progesterone, too, plays many roles in the body other than ovulation, including:
- Helps to support skin and bone health
- Supports pancreas function and normal insulin signalling
- Plays a role in regulating immune system function
It’s easy to see why the loss of these hormones trigger so many physiological changes, and why it can take some time for our bodies to adapt.
Health Conditions Associated with Menopause
With the significant physiological changes that occur in menopause, there are unfortunately an increased risk of certain other conditions developing in post-menopause.
High Cholesterol
After menopause, our bodies metabolise fats differently, which can unfortunately lead to an increase in “bad” LDL cholesterol and triglycerides.
Cardiovascular Disease
Low oestrogen increases the risk of CVD because of the protective role of oestrogen on the heart and blood vessels.
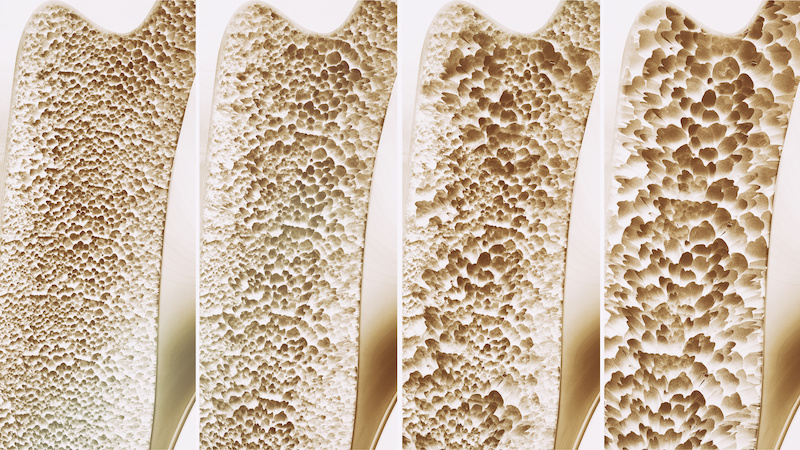
Osteoporosis
Our bones are living tissue, which is in a constant state of remodelling, thanks to specialised cells that break down bone to release minerals for use throughout the body, and then rebuild the bone again. This process is in part controlled by hormones, including oestrogen. Bone density is protected by oestrogen, so when oestrogen levels drop post-menopause, one of our protections against osteoporosis is lost, and bone loss can be quite rapid particularly in the first couple of years of menopause. Osteoporosis can have no symptoms for many years.
Metabolic Syndrome
Metabolic Syndrome is a collection of signs and symptoms that together increase the risk of other adverse health outcomes. The loss of both oestrogen and progesterone puts as at higher risk of developing Metabolic Syndrome. Signs, symptoms, and conditions associated with metabolic syndrome include:
- Impaired glucose metabolism – leading to high blood sugar
- High cholesterol and triglycerides
- High blood pressure
- Obesity
Weight Gain
Although not a health condition in itself, weight gain is a very common concern for post-menopausal women that shouldn’t be dismissed. Changes to hormones affect both metabolism and the way fat is stored in the body. Weight gain can begin during the perimenopausal period (the period 2-10 years before your period ends), and may continue after menopause, too. The weight gained during this time is often largely around the abdominal area and is due to the decline in oestrogen.
Insulin Resistance
Post-menopausal weight gain and the loss of progesterone can increase the risk of developing insulin resistance. Visceral fat – the kind that accumulates around abdominal organs – places additional strain on the liver because of the way it metabolises fatty acids. This extra strain on the liver can cause the liver to become insulin resistant.
Urinary Tract Infections and Thrush
UTIs can unfortunately rear their ugly head after menopause. Oestrogen is responsible for maintaining our vaginal secretions, pH and microbiome, which all act to protect against invading bacteria that cause UTIs.
Be aware that recurrent UTIs and thrush may also be a sign of other health issues, such as diabetes. If you are experiencing frequent UTIs or thrush, it is important that you seek advice so that further testing can be arranged if necessary.
Urinary Incontinence
Both oestrogen and progesterone are involved in maintaining healthy, toned muscles in the bladder and pelvis. Without this hormonal protection, muscle tone may be lost, leading to symptoms of urinary incontinence.
Sexual Wellbeing
Oestrogen is responsible for keeping the vagina lubricated and elastic. After menopause, the tissue of the vagina changes and can lead to dryness and painful intercourse. Some women may also experience reduced libido or sex drive, but others may not find this to be the case.
Ability to handle stress
With the loss of estrogen and progesterone, the ability to handle the same level of stress we once did is impacted. Women with senior careers and busy, demanding lives can feel this change in stress management ability quite significantly.
Looking After Yourself Post-Menopause

Diet
Eat Plenty of Vegetables and Fruits Daily
The antioxidants in vegetables and fruits protect against cardiovascular disease, while the fibre in these foods can help to lower blood pressure and keep our blood sugar levels in check, too. Fruits and vegetables also contain high amounts of anti-inflammatory compounds that are crucial for wellbeing after menopause. Aim for 2 serves of fruit and at least 5 serves of vegetables each day.
Reduce Your Intake of Red Meat
Red meat intake is associated with a higher incidence of heart disease. Additionally, and excess of certain protein can cause less calcium to be absorbed from food, leaving us at risk of calcium insufficiency and bone density issues. Keep red meat to no more than twice per week, and instead enjoy other protein sources such as fish, chicken, seafood, lentils and legumes, and soy.
Include Phytoestrogens in your Diet
Phytoestrogens are molecules found in many plant foods which can bind to oestrogen receptors in the body. Some examples of phytoestrogens include isoflavones and lignans. Phytoestrogens have a bad rap in Western culture as being damaging to our health, but this unfortunate misconception is due to a misunderstanding of how these molecules really work. Phytoestrogens have a “modulating” effect on oestrogen levels, so when oestrogen levels are low (such as in menopause), they can help to slightly increase oestrogen function in the body. Phytoestrogens can help to protect against bone mineral loss and osteoporosis, reduce hot flushes, and even reduce symptoms associated with vaginal dryness. Phytoestrogens can be found in a huge range of foods, including tofu, flax seeds, chickpeas, mung beans, olives, pumpkin seeds, parsley, buckwheat, and even whole grains.
Reduce Your Alcohol Consumption
Alcohol dilates blood vessels and increases luteinising hormone, which can make hot flushes worse. It can also be detrimental for sleep, which can be a particular concern after menopause. Alcohol is best avoided, but if you do choose to drink, stick to no more than 2 standard glasses one or two nights a week, and choose heart-healthy options such as red wine.
Reduce Your intake of Sugar
Added sugars in foods are a huge problem and high intake of sugar is associated with a number of health problems that are worsened after menopause, including heart disease and diabetes. Sugar intake can also be a big culprit when it comes to recurrent thrush. Always read labels and be aware of hidden added sugars in foods. Unexpected added sugar can be found in foods such as yoghurt, breakfast cereals, pasta sauce, peanut butter and other spreads, salad dressings, sauces, canned fruits, protein bars, bread, and even microwave meals.
Mediterranean Diet
The Mediterranean Diet is a fantastic eating plan for post-menopausal women, as it follows many of the above dietary recommendations. The evidence backs up its use, too. Studies have found it to be beneficial in reducing obesity and cardiovascular disease rates in postmenopausal women.
Individual Nutrients
Vitamin D and Calcium
Vitamin D and calcium regulate one another and are absolutely vital for strong bones.
To boost your vitamin D levels:
- Get daily sun exposure – 15 minutes of morning or late afternoon sun exposure is typically plenty.
- Foods – free range eggs, dairy, fortified foods
- Supplements may be necessary depending on your lifestyle, diet and current vitamin D levels
To boost your calcium levels:
- Sardines and other tinned fish
- Dark green leafy vegetables such as spinach, Bok choy and kale
- Tahini, tofu, legumes
- Note that while dairy has traditionally been promoted as the ideal high-calcium food, it is very high in protein, which can in fact put pressure on the kidneys and lead to an overall loss of calcium. This is why excessive protein intake is not a good idea, especially post-menopause. Be mindful of your protein and dairy intake and remember to include non-dairy calcium foods in your diet.
Omega 3 Fatty Acids
Omega 3 fatty acids are essential in our diet, because the body isn’t able to produce them. Omega 3 fatty acids are anti-inflammatory and can help to protect against developing cardiovascular disease and insulin resistance. Food sources of omega 3 fatty acids include nuts and seeds, fatty fish, flax seeds, walnuts, and soy. You may also benefit from a supplement but be aware that many over-the-counter omega-3 supplements are poor quality and may even contain rancid fish oil. Our clinic only prescribes the highest quality of practitioner only, clean fish oil supplements.
Probiotics & Prebiotics
A good quality probiotic supplement can make a big difference to your wellbeing after menopause if this is determined that this is what you need, particularly for maintaining vaginal health. Probiotic foods such as sauerkraut, Kim chi, and unsweetened Greek yoghurt can be great additions to your diet. Prebiotic supplements and foods are also helpful and our blog on sustaining healthy gut bacteria is here https://www.performanceinhealth.com.au/2020/06/11/microbiome-family-gut-health/
Lifestyle
Daily Weight-Bearing Exercise
Daily exercise is a must for good health post-menopause. Weight-bearing exercises such as walking, jogging, team sports like netball or hockey, are all great choices, as they help to promote bone density and protect against osteoporosis. Daily vigorous exercise of 30 minutes or more is good for more than just your physical health. It can also help to improve mental health, reducing anxiety and feelings of stress. Exercising outdoors in the mornings can also be an opportunity to get some vitamin D through sun exposure, as well as being good for your circadian rhythm (the body’s innate clock that helps us to sleep at night).
Quit Smoking
If you are a smoker, now is the time to quit. Smoking increases the risk of heart disease, stroke and high blood pressure. Whilst we can’t go back in time and increase our oestrogen levels, we can reduce our risk of heart disease by addressing these other, modifiable risk factors in our lifestyle.
Take Steps to Prevent UTIs
- Always wipe from front to back
- Urinate before and after sex
- Avoid wearing synthetic underwear or using douches and perfumed feminine hygiene products
- Shower and change your clothes after exercising
- Don’t ignore the urge to urinate
- Keep hydrated each day – around 2L
Keep Up to Date with Health Screening
There are a number of routine screening tests that you should keep up to date with as part of keeping healthy after menopause. These screening tests include:
- Mammograms
- Cervical smear (PAP smear)
- Osteoporosis risk assessment
- Heart disease risk assessment and blood pressure check
- Screen for bowel cancer
- Blood cholesterol testing
Put in place stress management & self-care strategies
This is a chapter in life where it is important to reduce stress and out in place ways to reduce cortisol, nurture the adrenals and commit to self-care each week for yourself. If this is neglected, you will feel it’s impact and your health will suffer.

Navigating this post-menopausal chapter with naturopathic guidance
For many women, this is in fact an empowering chapter of their lives. Whilst areas of negative changes are reflected above, it is also a time of significant emotional and mental well-being. Many women adore this stage of their lives. They are happier in their own skins and life can often become much more enjoyable. This aspect of menopause needs to be celebrated.
Whilst our risk factor for many diseases increase significantly after the loss of these precious hormones, it simply means that it is a time where you need to reassess how you do things.
A strategic review of your diet and may be something worth investing in, given the average weight gain at menopause is 12 kilos. Simple strategies can support you to make different choices.
Herbal medicine and supplement support
In my clinic, one of the most important priorities in supporting menopausal clients is to support and nurture adrenal health whilst providing guidance on a holistic approach to stress management. I do this with beautiful, gentle adrenal herbal medicines.
Higher cholesterol, blood sugar levels and weight gain can also be supported with some beautiful herbal remedies and dietary strategies.
Knowledge is power at this new female chapter, and I hope you find this blog valuable.
References
Ko, S.-H., & Kim, H.-S. (2020). Menopause-associated lipid metabolic disorders and foods beneficial for postmenopausal women. Nutrients, 12(202).
Lee, K., & Church, K. (2021, August 23). 5 health risks women face after menopause. https://www.everydayhealth.com/menopause/health-risks-women-face-after-menopause/
Mallorie, A., & Shine, B. (2022). Normal bone physiology, remodelling and its hormonal regulation. Surgery (Oxford), 40(3), 163–168.
Novella, S., Perez-Cremades, D., Mompeon, A., & Hermenegildo, C. (2019). Mechanisms underlying the influence of oestrogen on cardiovascular physiology in women. The Journal of Physiology, 597(19), 4873–4886.
Pugliese, G., Barrea, L., Laudisio, D., Aprano, S., Castellucci, B., Framondi, L., Di Matteo, R., Savastano, S., Colao, A., & Muscogiuri, G. (2020). Mediterranean diet as tool to manage obesity in menopause: A narrative review. Nutrition, 79–80.
Seifert-Klauss, V., Schmidmayer, M., Hobmaier, E., & Wimmer, T. (2012). Progesterone and bone: A closer link than previously realized. Climacteric, 15.
Trickey, R. (1998). Women, hormones and the menstrual cycle. Trickey Enterprises.
Walton, C., Godsland, I. F., Proudler, A. J., Wynn, V., & Stevenson, C. (1993). The effects of the menopause on insulin sensitivity, secretion and elimination in non-obese, healthy women. European Journal of Clinical Investigation, 23(8).